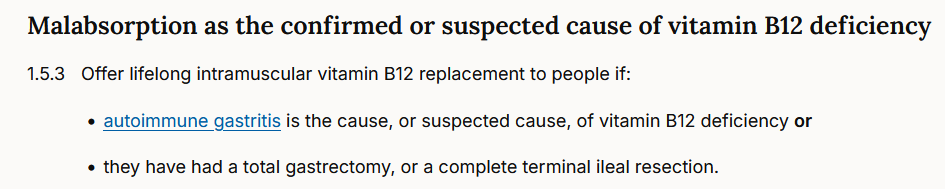
Ask any doctor which assay their laboratory uses for measuring auto-antibodies against intrinsic factor, and I am sure that over 95% of them do not have any clue. Yet, measuring IF antibodies plays an important role in the diagnosis of pernicious anaemia. The NICE guidelines state the following:

In November 2025, CluB-12 published three ‘Articles of the month’ on their website and in their monthly Newsletter. The reason for this selection was an email from a Dutch doctor stating, ”I only give B12 injections to people who are anaemic and have antibodies against intrinsic factor.”
Although vitamin B12 is an under-researched topic (which CluB-12 aims to correct), they selected the following three papers, in which the authors describe how they assessed the presence of IF antibodies in people with B12 deficiency.

What are the main findings of these papers?
In a study of 62 people with Biermer’s disease (another name for pernicious anaemia) in France (defined as B12 deficiency with either anaemia, atrophic gastritis, or severe neurological symptoms), 29 (47%) had detectable anti-IF antibodies when the authors used the DiaSorin assay (measurement method). When they repeated the measurements using other assays, such as those from Dxl, Aeskulisa, or BioAdvance, only 16, 12, and 12 people out of 62, respectively, tested positive for anti-IF antibodies.
A study in Poland included 124 people with proven pernicious anaemia. Of these, only 38 (30%) had antibodies to intrinsic factor (measured w. EliA, Thermo Fisher, Germany).
A study in Spain examined 5468 primary care patients out of whom 77 people had SEVERE vitamin B12 deficiency, defined as a serum B12 level below 74 pmol/L. A total of 44 patients (57%) had anti-parietal cell antibodies, whereas only 14% (11 of the 77) had antibodies to intrinsic factor (measured w. ELISA, Euroimmun, Germany). Worse still, only 32% had anaemia. The study does not mention the final diagnosis of these 77 unfortunate individuals. Given that around 1% of the population in Spain follows a plant-based diet, it is possible that some of these people had a B12 deficiency due to insufficient B12 intake, thus unrelated to the presence or absence of IF antibodies. Nevertheless, they all had a severe deficiency.
Key takeaway: Depending on the study, between 14 and 47% of people with PA had IF antibodies, but differences between assays may result in much lower percentages. The doctor who only treats people with B12 injections if they have anaemia with antibodies to intrinsic factor is, unfortunately, leaving many people with overt B12 deficiency untreated.
Links:
https://onlinelibrary.wiley.com/doi/epdf/10.1002/jcla.20272
https://www.degruyterbrill.com/document/doi/10.1515/cclm-2019-0749/html
https://www.mp.pl/paim/issue/article/15094/
It gets worse. A few weeks ago, a woman visited a medical specialist in the Netherlands. She was known to have pernicious anaemia, and had demonstrable auto-antibodies both against parietal cells and against intrinsic factor. Cause of the pernicious anaemia is, thus, autoimmune gastritis. Treatment with hydroxocobalamin injections according to the guidelines greatly reduced her symptoms. Yet, this medical specialist measured serum B12 and measured IF antibodies AGAIN. Serum B12 was high (PS. as is expected in people injecting B12) and IF antibodies were negative, so the advice was to stop B12 injections. The guidelines -reported above- are very clear, do not re-measure IF antibodies when they already tested positive on a previous occasion. It has been known for a couple of decades that high serum B12 in people injecting hydroxocobalamin may lead to false-negative IF antibody test results. Therefore, it is mandatory to do a good diagnostic work-up in people with pernicious anaemia BEFORE starting intramuscular B12 therapy. Testing again is throwing money out the window, as most laboratories charge between 40 and 60 Euro for such a test. No wonder that health care costs are increasing year after year….. lack of knowledge and unnecessary lab testing are expensive.
Also, stopping B12 injections in a person with demonstrated pernicious anaemia and B12 malabsorption is not the best advice, to say it politely. In pernicious anaemia, there is a very high risk of worsening or recurrence of symptoms when B12 injections are stopped, and even when people are forced to switch to oral supplementation. This is why the NICE guidelines are very explicit: lifelong intramuscular vitamin B12 therapy !
Stopping B12 therapy in people with pernicious anaemia is bad practice.
You can read all about this here: https://www.nice.org.uk/guidance/ng239
This article appeared previously in CluB-12’s November 2026 newsletter.
For translation into Dutch, copy this blog to Google Translate






Recente reacties